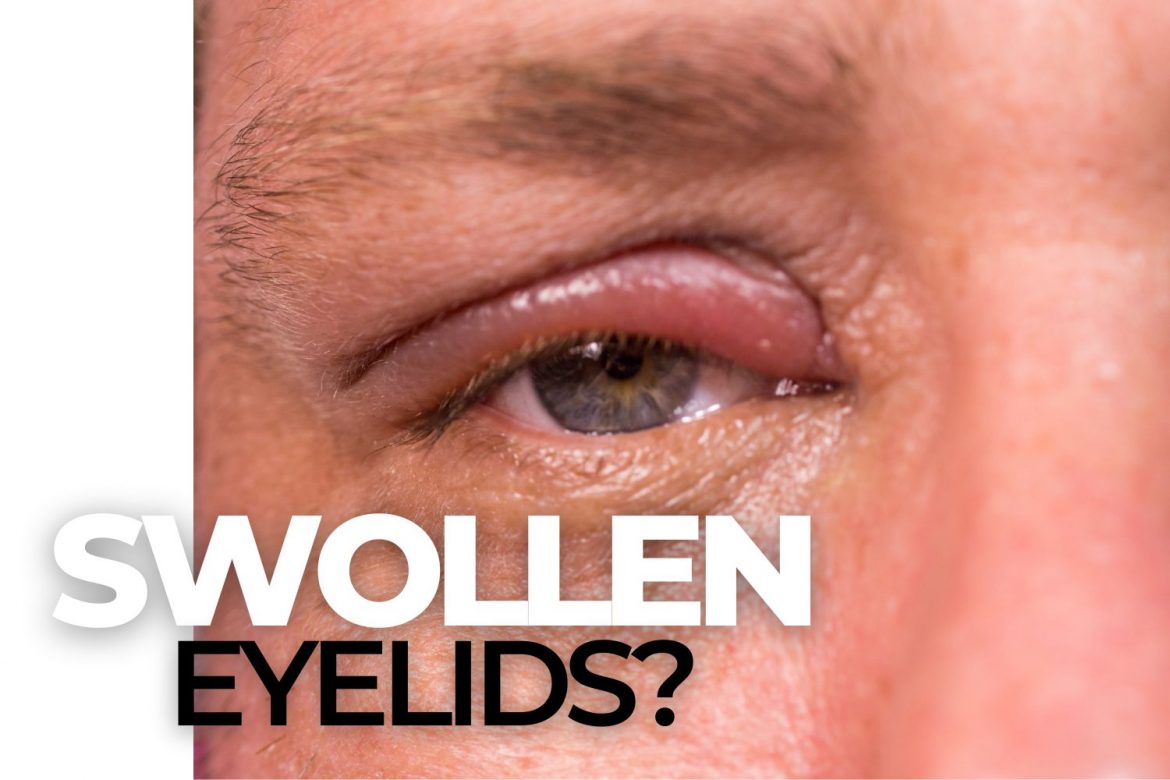
Do your eyelids ever look red, feel sticky, or sore? Do you have a constant itch in the corner of the eye that you just can’t scratch? Maybe it feels even worse when you wake up in the morning.
You may be one of the estimated 25 million Americans who suffer from blepharitis.
What is blepharitis?
Blepharitis is inflammation of the eyelid margin. Those who have blepharitis may have eyelids that appear red, swollen, or sore. Blepharitis is divided into two types: anterior and posterior, depending on the location.
- Anterior blepharitis refers to inflammation around the skin, eyelashes, and lash follicles.
- Posterior blepharitis affects the meibomian gland orifices, meibomian glands, tarsal plate, and blepharo-conjunctival junction (corner of the eyes).
Understanding blepharitis
Blepharitis is most often caused by staphylococcal bacteria but can be the result of a viral infection like Herpes simplex and Varicella zoster. It is diagnosed based on irritation of the lid margins and the presence of flaking and crusting of the eyelashes. Patient symptoms tend to be worse in the morning and unfortunately, it is typically a recurrent condition that affects both eyes over time.
Did you know mites live on your eyelashes?
Disgusting, huh? Yeah, what’s happening here is unpleasant…
Demodex folliculorum and Demodex brevis are two types of mites that infest the human eye and in abundance, can result in blepharitis. Demodex is a normal part of the flora that exists on the lid, and these mites are the most common microscopic ectoparasite on human skin.
Demodex infestation is underdiagnosed and undertreated. The mites are cigar-shaped with four pairs of legs to grip cylindrical objects like an eyelash, and mature from the egg to the larval stage in about two weeks. Their life span is up to three weeks.
Demodex folliculorum lives at the base of the lash follicle, where it feeds on epithelial (skin) cells resulting in damage. In addition to feeding, the mites lay their eggs at the base of the lashes resulting in detrimental changes in the eyelash follicle and misdirected lashes. These mites do not have excretory organs so undigested material is regurgitated and combine with these epithelial cells, keratin, and eggs to form the bulk of the deposits found on the eyelashes that cause eyelid irritation.
Demodex mites are found in both symptomatic and asymptomatic individuals and poor correlation exists between demodex infestation and symptoms.
Risk factors for blepharitis
A patient of any age can have blepharitis, but the risk increases with age. It can affect individuals of all ethnicities and genders. Patients who suffer from rosacea and seborrheic dermatitis are more likely to have blepharitis and it is often associated with other ocular conditions including dry eye, chalazion, conjunctivitis, and keratitis.
There is a distinct link between blepharitis and dry eye
Most dry eye is evaporative dry eye. Evaporative dry eye is due to a deficient tear film oil layer, which increases tear evaporation. The job of the oil layer is to balance the tear film. Increased evaporation is caused by meibomian gland dysfunction (MGD), which is estimated to be over 85% of dry eye disease. Blepharitis is both the cause and an effect of meibomian gland dysfunction.
Signs and symptoms of blepharitis
Blepharitis is diagnosed by an eye doctor based on the appearance of the eye and the patient’s symptoms. Common symptoms and signs of blepharitis may include:
- Burning
- Irritation
- Tearing
- Light sensitivity (photophobia)
- Blurred vision
- Red eyes
- Itchy eyelids
- Eyelid hyperemia
- Loss of eyelashes
The signs of blepharitis can be observed when a doctor looks at the front of the eye using a microscope called a slit lamp. Patients with the condition may have scurf on the eyelashes, new blood vessel changes on the eyelid margin, clogged meibomian glands, red eye, and signs of inflammation on the cornea.
While it is rarely a sight-threatening condition, chronic blepharitis may cause keratitis and corneal ulcers which result in vision loss.
Treatment for blepharitis
Blepharitis can be challenging to treat and manage because it tends to be a chronic condition. The main treatment is good eyelid hygiene to reduce the symptoms and prevent a recurrence. Therapy includes warm compresses, lid scrubs, and artificial tears. More advanced cases may require treatments like anti-inflammatory drops (steroids) or cyclosporin A. Often, a combination of topical antibiotics and oral antibiotics may be indicated.
Warm compresses
A washcloth can be heated with warm water and held at the base of the eyelashes. A device like a Bruder mask may be recommended over a warm washcloth because it holds the heat for longer periods of time. Warm compresses work by warming the oil inside the glands and loosening the flakes around your eyelashes. In-office devices may also be used by your eye doctor.
Eyelid scrubs
Eyelid scrubs are recommended for keeping the lids clean and clear. Bacteria are always present on the skin and eyelashes, but eyelid scrubs reduce bacterial load. Baby shampoo diluted with warm water can be used to scrub the eyelashes or your doctor may recommend a specific brand of OTC wipes like Ocusoft.
Eye drops
Artificial tears or steroid eye drops may be recommended to treat the associated dry eye. Dry eye is inflammation on the surface of the eye and depending upon the stage, treatment may include both types of eye drops.
Antibiotics
Ointment, topical drops, or an oral antibiotic may be prescribed by your doctor. The class of antibiotics called tetracyclines has shown promising results in treating blepharitis as the drug has both anti-bacterial and anti-inflammatory properties.
Demodex blepharitis can be difficult to treat because traditional methods fail to eradicate the mites. Treatment and management typically include a combination of lid scrubs and the removal of the eyelash collarettes with the use of a blepharitis brush or a cotton-tipped applicator and lid foam. Tea tree oil is currently the go-to in-office and at-home treatment option for demodex. Patients diagnosed with demodex are typically prescribed an eyelid cleanser that contains tea tree oil to be used twice daily to smother the mites.
Blepharitis is a common, chronic condition that affects millions of people each year. It can be frustrating and difficult to manage because it requires daily lid hygiene. The goal of treatment is to reduce eye symptoms and prevent reoccurrence. Most significantly, blepharitis can lead to long-term damage to the skin of the lids, the structure of the eyelashes, and the meibomian glands at the base of the eyelashes resulting in dry eye disease.