According to the American Optometric Association (AOA), dry eye is a diagnosis with which a person has inadequate tears available to lubricate the eye.
Tears comprise a mixture of water, fatty oils and mucus that maintain the smoothness and clarity of vision while preventing the risk of eye infections. When the tear ducts do not provide the regulation of tear lubrication, patients experience constant irritation, burning, excessive tearing and blurred vision. With each blink of an eye, tears provide nourishment across the entire surface of the cornea and wash away foreign matter.
Causes and symptoms of dry eye syndrome
A common cause of dry eye syndrome, as explained by the National Eye Institute (NEI) is decreased tear production, known as keratoconjunctivitis sicca (KCS) in clinical terms.
This condition is characterized by dryness of the conjunctiva (the membrane that covers the sclera, the white part of the eye, and lines the eyelids) and the cornea (the layer in front of the iris and pupil). The inability to produce enough tears is usually caused by aging, systemic diseases, medications, and refractive surgery.
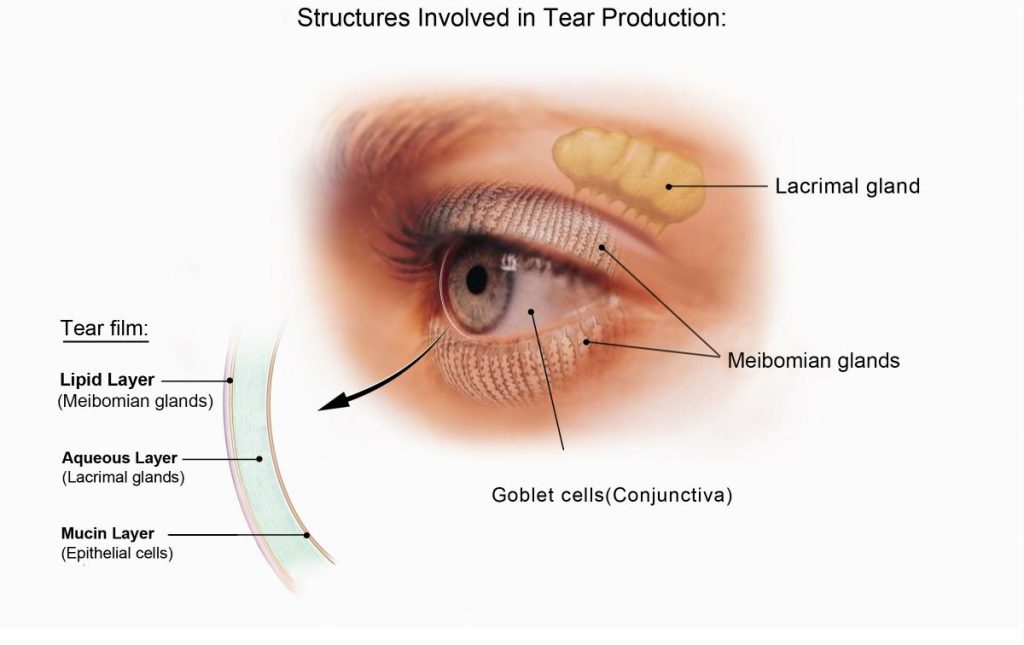
A number of medical conditions often cause dry eye syndrome including:
- Diabetes: Diabetic patients commonly
experience burning and a foreign body sensation. Additional findings include
unsteady tear film production,
reduced corneal feeling and decreased lipid layer in the tear film. Other
studies show a higher grade of conjunctival squamous metaplasia (change in the
epithelium cells to a squamous appearance) and lower goblet density (an
epithelial cell that plays a role in maintaining the ocular surface).
- Rheumatoid arthritis: Although this inflammatory disease
primarily affects the joints, it can cause dryness. Rheumatoid arthritis can lead
to scleritis, inflammation of the sclera, which eventually results in redness,
aching and possible changes in vision.
- Lupus: This systemic autoimmune disease
usually affects different parts of the body, including the eye. Lupus can cause
a change in the skin around the eyelids, dryness of the corneal surface,
scleritis, changes in the blood vessels in the retina, and damage to the nerves
in the eye muscles that control eye movement. Approximately 20% of Lupus
patients tend to develop Sjogren’s syndrome, secondary to the autoimmune
disease.
- Sjogren’s Syndrome:
Primary Sjogren’s syndrome, like Lupus, affects many parts of the body. Secondary
Sjogren’s syndrome affects the eyes, where the glands are inflamed and in turn
reduce tear production and result in chronic dryness. Thin spots of dryness may
show in the tear film where tears no longer are able to protect and lubricate.
- Thyroid Disease: Symptoms of thyroid eye disease may
occur in patients who are already aware of their disease, or it may be the
first indication that brings the patient to the eye doctor. The main symptoms
of thyroid eye disease are bulging eyes, dryness, excessive tearing, redness,
double vision, and difficulty closing the eyes (which leads to more dryness).
- Vitamin A deficiency: Vitamin A assists in protecting the surface of the eye with mucous membrane acting as a barrier against eye infections. As a result, Vitamin A is beneficial for the maintenance of good vision. Vitamin A eye drops have been shown to be effective in the treatment of superior limbic keratoconjunctivitis (SLK), a specific type of inflammation of the eyes; SLK symptoms are usually burning, irritation and redness.

Some medications are known to cause dry eyes
- Acne medication: This has a drying effect on the oil
glands known to irritate the eyes and eyelids. Acne medication is known to decrease
overall mucus production and secretion.
- Antidepressants: These medications block the
transmission of nerve impulses which make it difficult to sense dryness of the
eyes.
- Antihistamines: Although they hinder the effect of
histamine and provide relief against allergy and cold symptoms, they reduce the
watery tear film that lubricates the eyes. The effect of antihistamines is
ironic as it can produce eye symptoms similar to that of allergies.
- Birth control: Due to hormonal changes from the
drugs, dry eyes are a common risk taken with birth control.
- Cholesterol-lowering drugs: Among many other changes in the
body, statins have been linked to dry eyes.
- Decongestants: Like antihistamines, they decrease
tear production in the eyes.
- Eye drops: Certain eye drops for red eyes are known to make dry eye symptoms worse. The drops narrow the blood vessels to reduce redness, but when the drops wear off the vessels become larger and more inflamed. Allergy eye drops are also risky, because the patient may not know the true cause of the itchy eyes; the itching may be a symptom from dryness, which doesn’t solve the root of the problem.

- Diuretics: They reduce the tear production in
the eyes and cause dry eye.
- Hormone replacement therapy: There is a strong correlation of
increased risk of dry eye with women taking hormone therapy, due to their
hormonal changes; the medication has been known to affect the oil-producing
glands and reduce the water layer of the tear film.
- Hypertension drugs: They are known to decrease
sensitivity to the cornea, affecting the stimulus for the lacrimal glands.
- Parkinson’s disease medication: This medication has the same
anticholinergic property as antidepressants and antipsychotic drugs, also known
to block the transmission of nerve impulses. PD patients tend to blink only 1-2
time per minute (as opposed to 16-18 times), leading to dryness, irritation and
burning.
The lists of systemic disease and medications reiterate the importance of eye health, as people tend to forget its important role in the body. Depending on the severity of the dryness, an optometrist or ophthalmologist can determine which type of treatment to take for the patient’s specific needs.
Common treatment methods for dry eyes
- Artificial tears: Over-the-counter lubricating eye
drops with low viscosity provide quick relief with minimal (temporary) blurring
of the vision when applied. Drops with a higher viscosity are usually gel-like
and provide longer-lasting lubrication with blurry vision for a few minutes.
- Restasis: An alternative to the preservatives
in OTC artificial tears, this is a prescription eye drop that reduces
inflammation. It is crucial to use the drops twice a day for a minimum of 3
months to take full effect of its benefits.
- Xiidra: A relatively newer vision of
Restasis, this is also a prescription eye drop instructed to use twice a day
for at least 12 weeks before results can be shown.
- Punctal plugs: The small sterile plugs get inserted
into the lower tear duct to retain the eye’s moisture from draining away too
quickly. There are two kinds of punctal plugs: dissolvable ones, or ones that
remain in the ducts until they need to be replaced again (from falling out).
- Warm compresses: This inexpensive way to express the clogged meibomian glands that contain hardened oil glands does not work for everyone. Relief depends on the severity of the tear film reduction and the temperature of the heat from the warm compresses. In fact, this method is discouraging as it is recommended to keep the compresses constant for about ten minutes each time. After a while, people tend to lose this routine.
- Supplements: Omega-3 fatty acids have been
studied to decrease dry eye symptoms, which can be found in fish, flaxseed oil
(a vegetarian source), and fish supplements.
- Water: Drinking more water may help reduce the symptoms of dry eye syndrome.
Many internal and external changes in the body and environment play a role in the health of the eye. It is important to regularly visit your primary physician to find out the root of the problem before finding over-the-counter remedies for your eye problems.
If your dry eye symptoms persist, it’s crucial to visit your eye doctor. The above-mentioned pointers are for the overall education of the patient to bring awareness of the direct correlation of medicine, disease and dry eye effects.